It's been called a "demographic watershed".
In the next 15 years alone, the worldwide population of individuals aged 65 and older is projected to increase more than 60%, from 617 million to about 1 billion.1
Increasingly, countries are asking themselves: How can we ensure a high quality of care for our growing aging population while keeping our healthcare costs under control?
The answer? More efficiency. Less waste. Reduced error. Quicker turnaround. Improved patient outcomes. Which is, of course, where lean/six sigma quality improvement comes in.
Another Watershed: Lean/Six Sigma in Healthcare
Faced with the challenge of increased demand and rapidly rising cost, it's no surprise that more and more lean and six sigma studies are being performed and published in the fields of medicine and healthcare. A search for "lean sigma" or "six sigma" in the U.S. National Library of Medicine/National Institutes of Health database pulls up over 470 published studies. The year-by-year search results are shown in the following Trend Analysis Plot in Minitab.
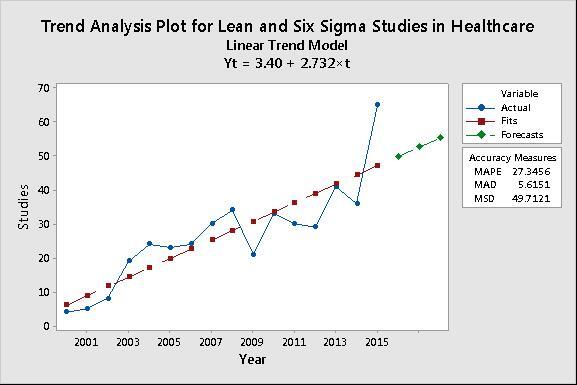
Note that this trend forecast based on a linear model could be conservative. The database already shows 39 published studies in the first 6 months of this year (2016). In the coming years, these data may require a quadratic (curved) model!
A Surprising Breadth of Applications
QI studies in healthcare run the gamut. Reducing appointment no-shows. Avoiding preventable hospital readmissions. Cutting down on the amount of expired medical drugs and equipment that must be discarded. Reducing the number of falls in nursing care facilities. Even tracking and reducing the number of times the door is opened and closed during surgeries!
The one consensus in all these diverse studies? There's no shortage of opportunity for trimming waste and for improving patient outcomes in the healthcare setting.
Improving on Improvement: Statistical "Soft Spots"
With the increased number of published studies in lean/six sigma healthcare, comes increased scrutiny. Review studies are beginning to look more closely at the methods used to monitor and measure healthcare quality outcomes. These reviews have identified statistical shortcomings in the published studies.2-4
-
No testing for statistical significance
A study might report a reduction in, say, mean waiting times for surgery for patients after an improvement initiative. But no statistical analyses are performed to determine whether that reduction is statistically significant. -
Lack of randomization
The samples examined in a study are not randomly selected, and may not be representative of the population. Therefore, the results are subject to selection bias. -
Inadequate follow-up
A study might report a statistically significant change after a lean/six sigma initiative, but there is lack of adequate follow-up. Therefore, it's unclear whether the improvement "stuck" or whether the initial change was simply a short-term Hawthorne effect. -
Missing confidence intervals
Many studies neglect to report associated confidence intervals with their results. As a result, the level of precision is unclear, and the clinical significance of the results cannot be reliably interpreted.
No Single Study is a Statistical Slam-Dunk
There's no such thing as a "perfect" study. You do the best you can, with the resources you have and the constraints you face. Progress is made in increments. Conditions change. And results must be re-verified and reproduced.
Still, it's important to remember that "continuous improvement" can be applied not only to the process itself, but to the methods that we use to monitor and improve a process. To get the most out of quality improvement efforts in healthcare, it's critical to be aware of the common statistical soft spots, and how to avoid them.
That way, when the wave breaks, we'll be on sturdier ground.
Sources
1 An Aging World: 2015. International Population Reports. US Census Bureau. Available here.
2 Nicolay CR, Purkayastha S, Greenhalgh A, Benn J, Chaturvedi S, Phillips N, Darzi A . Systematic review of the application of quality improvement methodologies from the manufacturing industry to surgical healthcare. Br J Surg. 2012 Mar;99(3):324-35. 2011 Nov 18.
3 Amaratunga T, Dobranowski J. Systematic review of the application of Lean and Six Sigma quality improvement methodologies in radiology. J Am Coll Radiol. 2016 May 18.
4 Mason SE, Nicolay CR, Darzi A. The use of Lean and Six Sigma methodologies in surgery: a systematic review. Surgeon. 2015 Apr;13(2):91-100.
Photo: Big Wave Breaking by Brocken Inaglory. Licensed by Wikimedia Commons.



